According to the WHO, 1 in 10 patients worldwide experiences harm during healthcare, resulting in over three million deaths annually. Notably, more than 50% of these adverse events (1 in every 20 patients) are preventable, with medication-related errors accounting for a large portion. Incident reporting in healthcare plays a crucial role in spotting and reducing the risks that threaten patient safety.
This article will explore how an effective incident reporting system in healthcare enhances care quality, promotes a culture of transparency, and drives continuous improvement.
- What is Incident Reporting in Healthcare?
- Examples of Incident Reports in Healthcare
- Incident Reporting Process in Healthcare Settings
- Simplify the Incident Reporting Process with GoAudits
- Free & Customizable Checklists to Ensure Patient Safety
- Key Elements of an Incident Reporting System in Healthcare
- Barriers to Incident Reporting in Healthcare
- How to Improve Incident Reporting in Healthcare
- FAQs
What is Incident Reporting in Healthcare?
An incident report is a comprehensive record of an unexpected occurrence within a healthcare setting. This includes detailing the incident’s nature, the individuals involved, and the resulting outcomes. The primary purpose of such reporting is to capture accurate information about incidents to facilitate analysis, identify underlying causes, and implement corrective actions to prevent future occurrences.
Types of Incident Reports in Healthcare
Incident reports in healthcare can be categorized into several types, each addressing different aspects of patient and staff safety:
- Clinical Incidents: These involve events directly related to patient care that result in, or have the potential to result in, harm. Examples include medication errors, surgical complications, or misdiagnoses.
- Sentinel Events: These are serious incidents that result in severe patient harm or death. These events require immediate investigation and root cause analysis. Examples include wrong-site surgery, patient suicide within a healthcare facility, or administering the wrong medication, leading to fatal outcomes.
- Near Miss Incidents: Situations where an error occurred but was identified and corrected before causing harm. Reporting near misses in healthcare is crucial as it helps in identifying system vulnerabilities and preventing future adverse events.
- Non-Clinical Incidents: Events not directly related to patient care but occurring within the healthcare environment. This includes equipment failures, infrastructure issues, or administrative errors.
- Workplace Incidents: Incidents affecting healthcare staff, such as occupational injuries, exposure to hazardous substances, or instances of workplace violence.
Importance of Incident Reporting in Healthcare
Incident reporting can help healthcare organizations identify and address underlying issues, preventing future occurrences. Here are the major benefits of incident reporting in healthcare:
- Helps identify errors and apply corrective actions to continuously improve patient care standards.
- Detects incident patterns, enabling proactive clinical risk management and safer healthcare environments.
- Learning from reported incidents helps prevent harm and improve overall patient outcomes.
- Encourages open reporting and provides a clear view of system performance and improvement areas.
- Increases staff awareness of risks and promotes adherence to best practices.
- Ensures healthcare organizations meet legal and regulatory reporting requirements.
- Incident documentation and analysis help prevent similar events in the future.
Examples of Incident Reports in Healthcare
In healthcare settings, common incidents that require detailed reporting include:
Medication Errors
Medication-related incidents are among the most frequently reported in healthcare. These errors include administering the wrong dose, providing medication to the wrong patient, or omitting a prescribed dose.
For example, a nurse might scan a medication barcode, become distracted, and then inadvertently administer the wrong medication.
Patient Falls
Patient falls are unexpected events that can significantly impact patient safety, often resulting in injuries such as fractures, lacerations, or internal bleeding. These incidents necessitate documentation to outline the events leading up to and following the fall.
For instance, a patient slipping on a wet floor near the nurse’s station would require an incident report detailing the circumstances and any subsequent injuries.
Surgical Complications
Surgical procedures carry inherent risks, and complications can arise due to human error, equipment failure, or unforeseen circumstances. Incidents such as retained surgical instruments or wrong-site surgeries require thorough reporting to analyze the entire surgical process and prevent future occurrences.
For example, a patient experiencing an unexpected postoperative complication following a routine surgery would prompt an incident report to investigate potential systemic flaws.
Communication Issues
Effective communication is essential as breakdowns can lead to significant incidents. Miscommunication of drug orders, illegible handwriting, or confusion over similarly named drugs can result in medication errors.
For instance, a failure to communicate a critical lab result to the attending physician could adversely affect patient care, necessitating an incident report to address the communication lapse.
Patient Misidentification
Accurate patient identification is essential to ensure appropriate care. Errors such as administering treatment to the wrong patient due to misidentification can have serious consequences.
For example, a patient receiving another’s medication because of a mix-up in identification bands would require an incident report to investigate and rectify the identification procedures.
👉 Free Resources
Incident Reporting Process in Healthcare Settings
Here’s a step-by-step guide to simplify the incident reporting process:
1. Identify and Document the Incident
Promptly recognizing and accurately documenting any unexpected event includes detailing the incident’s nature, time, location, individuals involved, and any immediate actions taken. Comprehensive documentation ensures that all pertinent information is captured while it remains fresh.
2. Submit the Report
After documentation, submit the incident report through the designated channels within your healthcare facility. Timely submission ensures the review process is initiated promptly and corrective actions are taken. The report should be clear, concise, and free from personal opinions to maintain objectivity.
3. Review and Analyze
Once submitted, the incident report is reviewed by the appropriate personnel or committees to identify the root causes of the incident, assess its impact, and determine contributing factors. A detailed review is essential for understanding the underlying issues and preventing recurrence.
4. Conduct Root Cause Analysis
Root cause analysis (RCA) helps healthcare organizations determine the underlying causes of an incident rather than focusing only on the immediate issue. Techniques such as the 5 Whys method or fishbone diagrams are commonly used to identify systemic problems.
5. Take Corrective Action
Based on the findings from the analysis, implement corrective measures to address the identified issues. These actions may involve revising protocols, enhancing training programs, or introducing new safety procedures to mitigate risks and prevent similar incidents in the future.
6. Follow Up
After implementing corrective actions, conduct follow-up evaluations to ensure their effectiveness. This may include monitoring compliance, assessing outcomes, and gathering feedback from staff. Continuous monitoring helps in identifying any gaps and making necessary adjustments.
7. Learn, Improve, and Update
Regularly review and update policies, procedures, and training materials based on insights gained from incident reports. Fostering a culture of learning and openness encourages staff to report incidents without fear of retribution, enhancing overall patient safety.
Simplify the Incident Reporting Process with GoAudits
GoAudits healthcare compliance software can help healthcare professionals streamline incident reporting and auditing processes, improving workplace safety, compliance, and accountability. Accessible via the web, iOS, and Android devices, it helps them capture and track incidents in real-time. GoAudits also enables them to quickly address issues, assign corrective actions, and improve operational efficiency.
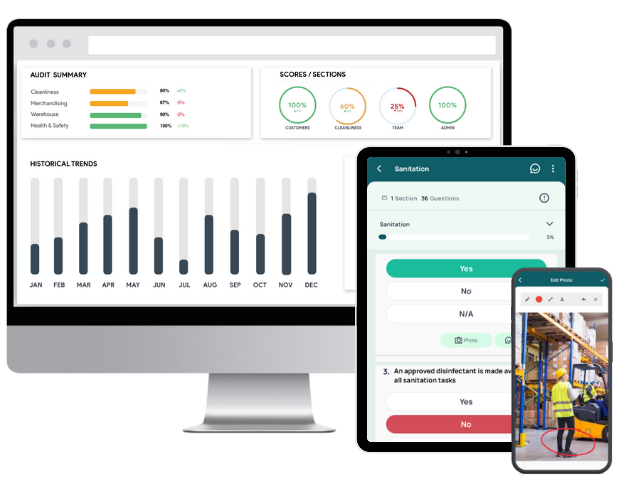
- Conduct audits and report incidents directly via mobile, whether online or offline.
- Generate and share incident reports instantly in a branded, visual format.
- Customizable templates ensure all necessary details are captured, improving accuracy and efficiency.
- Automatically assign corrective actions, tasks, and approvals with clear deadlines and priorities.
- Ensures no task slips through the cracks, reducing delays and improving resolution times.
- Interactive dashboards provide real-time insights into incident trends and resolutions.
- Helps teams track progress, identify recurring issues, and take proactive steps.
- Set up specific roles and permissions within the app to control access and reporting.
Free & Customizable Checklists to Ensure Patient Safety
GoAudits offers a wide range of audit checklists for different healthcare facilities. You can sign up for free and use these checklists to prevent and report incidents and ensure patient safety.
- Monthly Accident & Incident Audit
- Weekly Accident Audit
- Elderly Fall Prevention Checklist
- Patient Fall Risk Assessment
- Monthly Fire Safety Inspection
- Workplace Safety Audit Checklist
- Nursing Home Safety Checklist
- Medication Audit Checklist
- Home Safety Assessment for the Elderly
- Care Home Safety Checklist
Key Elements of an Incident Reporting System in Healthcare
To ensure comprehensive documentation and facilitate meaningful analysis, it’s essential to include the following key elements:
Basic Information
Begin with essential details such as the date, time, and location of the incident. It helps in contextualizing the event and aids in identifying patterns over time.
Individuals Involved
Clearly identify all parties involved, including patients, healthcare providers, and any other personnel. It ensures accountability and assists in understanding the roles each individual played in the incident.
Detailed Description of the Incident
Provide a factual and thorough account of the incident, outlining the sequence of events leading up to it. Avoid subjective language to maintain objectivity, which is crucial for accurate analysis.
Type of Incident
Specify the nature of the incident, such as medication errors, patient falls, or equipment malfunctions. Categorizing incidents helps in identifying common issues and areas requiring improvement.
Immediate Actions Taken
Document the steps taken immediately following the incident to mitigate harm and address the situation. This information is essential for assessing the effectiveness of the response and for future reference.
Witness Statements
Include statements from individuals who witnessed the incident. Witness accounts can provide additional perspectives and may reveal contributing factors not initially apparent.
Contributing Factors
Identify any underlying issues that may have contributed to the incident, such as staffing shortages, equipment failures, or communication breakdowns. Recognizing these factors is essential for implementing effective preventive measures.
Outcome and Impact
Describe the consequences of the incident, including any harm to patients or staff, and the impact on operations. Understanding the severity of the outcome is crucial for determining the necessary corrective actions.
Preventive Measures
Outline strategies implemented to prevent similar incidents in the future. This may include staff training, policy revisions, or equipment upgrades. Documenting these measures demonstrates a commitment to continuous improvement.
Reporting Personnel Information
Record the details of the individual reporting the incident, ensuring they are identifiable. This information is important for follow-up and for maintaining a transparent reporting process.
Follow-Up Actions
Detail any subsequent actions taken to address the incident, such as investigations, disciplinary measures, or changes in procedures. Follow-up actions are essential for closing the loop and ensuring that lessons are learned.
Barriers to Incident Reporting in Healthcare
Several barriers can impede the incident reporting process in healthcare, including the following:
- Lack of Feedback: When healthcare professionals report incidents but receive no feedback, they may feel their efforts are futile. It can lead to disengagement and a reluctance to report future incidents.
- Complex Reporting Systems: Intricate and time-consuming reporting procedures can discourage staff from reporting incidents.
- Perceived Futility: Some healthcare professionals believe that reporting incidents will not lead to meaningful change. This perception can stem from a history of unaddressed issues or a lack of visible improvements.
- Lack of Awareness: Insufficient training and awareness about the importance and procedures of incident reporting can hinder participation.
- Fear of Blame or Punishment: A culture of blame can deter individuals from reporting incidents due to fear of retribution.
- Lack of Interdisciplinary Cooperation: Effective incident reporting often requires collaboration across various healthcare disciplines. A lack of interdisciplinary cooperation can impede the reporting process.
- Time Constraints: Healthcare professionals often face demanding schedules, leaving little time for incident reporting.
- Incident Forms Take Too Long to Complete: Lengthy and detailed incident reporting forms can deter healthcare professionals from reporting incidents.
How to Improve Incident Reporting in Healthcare
Implementing the following strategies can help overcome the above challenges and lead to significant improvements:
Create a User-Friendly Reporting System
Develop an intuitive and accessible reporting system that encourages healthcare professionals to report incidents without hesitation. A straightforward process ensures that staff can easily document adverse events and near misses.
Foster a Blame-Free Culture
Cultivate an environment where staff feel safe to report incidents without fear of retribution. A blame-free culture promotes transparency and encourages open communication.
Provide Training and Education
Offer regular training sessions to educate staff on the importance of incident reporting and the proper procedures to follow. Well-informed staff are more likely to engage in reporting.
Ensure Prompt Feedback and Follow-Up
After an incident is reported, provide timely feedback to the reporting individual and the team. This practice demonstrates that their input is valued and leads to continuous improvement in patient safety.
Simplify the Reporting Process
Use incident reporting apps to streamline the reporting process and reduce complexity and time requirements. An efficient system encourages more frequent reporting and ensures that incidents are documented accurately.
Use Healthcare Data to Identify Trends
Analyze collected incident data to identify recurring issues and trends. This enables healthcare organizations to implement targeted interventions to address systemic problems and enhance patient safety.
Regularly Communicate Outcomes
Share the outcomes of reported incidents and the actions taken to address them with all staff members. Regular communication fosters a sense of collective responsibility and keeps everyone informed about ongoing safety initiatives.
FAQs
These terms are often used interchangeably in healthcare settings. Both refer to the documentation of occurrences that deviate from standard procedures or expectations. However, they can be different in some aspects. Event reporting includes a broad range of occurrences, including both adverse events and near misses. Incident reporting typically focuses on specific incidents that have resulted in harm or had the potential to cause harm.
Any healthcare professional who witnesses or is directly involved in an incident should complete the report. This can include nurses, physicians, pharmacists, or support staff.
An incident report should be filed as soon as possible after the event occurs, ideally immediately after patient safety is secured. Prompt reporting ensures accurate documentation while details are fresh and allows healthcare teams to investigate the incident and implement corrective actions quickly.
Yes, incident reports are typically treated as confidential internal documents. Access is usually limited to authorized personnel involved in reviewing and investigating incidents, ensuring sensitive information about patients and staff is protected.
Hospitals commonly report clinical incidents, near misses, medication errors, workplace injuries, patient identification errors, and equipment malfunctions. Reporting these incidents helps healthcare organizations analyze safety risks and improve patient care systems.
Accurate reporting requires documenting factual details immediately after the incident, avoiding assumptions, and including timelines, actions taken, and contributing factors. Digital incident reporting platforms like GoAudits help healthcare teams capture accurate data, assign corrective actions, and track safety improvements in real time.
Digital tools simplify incident documentation, automate reporting workflows, and provide real-time safety insights. GoAudits allows healthcare teams to report incidents from mobile devices, assign corrective actions, monitor trends, and ensure safety issues are addressed quickly across facilities.





